Risk Factors of Suicide: the conventional list, and perspective from a biological researcher
When someone attempts or dies by suicide, many of us are inclined to ask ‘why?,’ but often there is no particular answer.
Suicide is a complex phenomenon, with evidence of contributing influences encompassing social, genetic, familial, neurobiological, economic, neuropsychological, environmental, and situational factors. There is no singular ‘cause’ of suicide, but years of research have resulted in lists of risk factors—characteristics that are associated with an increased chance of suicidal behavior. Some researchers divide these risks into predisposing or distal (i.e. historical contributors, such as genetics, early trauma, or chronic illness) or precipitating or proximal (i.e. recent or precipitous triggers, such as a job loss or recent illness.)
Psychological conditions are high on this list, and these range from diagnosed disorders such as depression and psychosis; to substance use, eating and personality disorders; to personality characteristics such as impulsivity and aggression. While mood disorders and depression are often more highly associated with ideation, research has shown that suicidal action correlates more directly with anxiety and panic disorders. Chronic illness, family history, abuse or trauma, and access to lethal means also raise risks.
Most of these factors are common and relatively stable conditions, and the majority of those with these exposures will not consider or attempt suicide. Suicide impulses can change day-to-day or even in a matter of minutes; for some, they can subside as quickly as they present but for others the ideation can be ongoing. At least in the moment, suicide is the result of disordered thinking that reduces an individual’s ability to problem-solve and see other options, and overtakes instincts of self-preservation.
Hard to predict risk in any given individual
Since established risk factors are not specific regarding whom or when, it is difficult to predict either short- or long-term risk, making timely intervention challenging for therapists and doctors, as well as for loved ones. Much of our knowledge of risk factors comes from learning from survivors of suicide attempts and ‘psychological autopsies’ performed after a suicide, but we only know the answers to the questions we have asked–most of which have concentrated on a person’s psychosocial history–mental state, trauma, and social environment.
A 2017 comprehensive study covering the past 50 years of suicide research found that we still don’t know what matters; it remains difficult to predict risk beyond chance and half of all suicides are in those considered low risk. With virtually no historical evaluation of multi-factorial risk scenarios, the authors suggest a shift in research focus to machine learning-based algorithms and large biological risk factor studies.
This is the kind of novel thinking we are interested in at JKBF, in the hopes that looking at factors beyond psychosocial elements might reveal new opportunities for treatments and preventive measures.
Novel insights on risk from a biological researcher

Recently JKBF hosted a small group of community members for an intimate presentation generously provided by Teodor Postolache, MD. Dr. Postolache, a licensed and practicing board-certified psychiatrist, Professor of Psychiatry at University Of Maryland, and Research Investigator with the Department of Veteran’s Affairs, treats patients with mood, anxiety, and seasonal affective disorders. Employing a head-to-toes approach with consideration of the physical, chemical, and biological environment in his treatment of each patient, he also applies this multi-disciplinary approach to research.
In his talk entitled Immune-mediated Risk Factors for Suicide Behavior Dr. Postolache shared elements of his approach to both treatment and research, and his focus on identifying reversible and modifiable factors. Dr. Postolache makes the argument that virtually every factor, psychosocial as well as measurable physiological, is biological.
As a clinician, Dr. Postolache noticed that most of his patients have rhythms of intensity of mood disorders and/or heightened suicide risk. For some this cycle might have psychosocial origins, such as the anniversary of a loss or trauma. But for others, these cycles might relate to menstrual cycles or seasons–factors that are more biological. Dr. Postolache responds to these cycles by concentrating psychiatric care during those times of highest risk, but also started exploring biological clues.
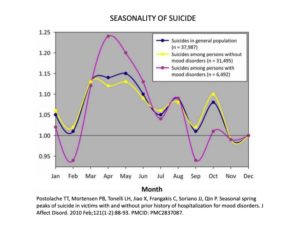
Worldwide historical data showing seasonal spring spikes in suicide led him to investigate the possibility that exposure to seasonal allergens might increase risk. While there is still more work to be done to replicate and explore possible mechanisms, Dr. Postolache’s early findings of an association (see graph) between allergen exposure and suicide rates got significant attention and helps to shift our thinking.
With other biological research showing that stress and trauma promote inflammation, the role of the immune system in psychiatric concerns and suicide is of great interest to Dr. Postolache and his collaborators. They note that treatment of certain illnesses with drugs that promote inflammation can make patients depressed and increase suicide attempts and deaths. Conversely, anti-inflammatory treatments, such as those applied in auto-immune disorders, appear to be protective. While the immune system does a lot of good, sometimes an overabundance of immune molecules, called cytokines, can create harm as well.
Bi-directionality
We tend to think of the mind and body as distinct, but Dr. Postolache highlights that bi-directionality has to be considered. Stress can be a trigger and a consequence of inflammation, and pathways that connect the brain to the body (and vice versa) are worth exploring: the blood brain barrier, the vagal nerve, and intranasal channels.
In addition, illness can affect our mood, thinking, and behavior. Dr. Postolache has published on suicide risk being increased with the parasite Toxoplasma gondii, generally considered to be harmful if acquired during pregnancy but otherwise relatively benign as a chronic infection. Perhaps not, as research shows that infection changes the behavioral characteristics of mice, who become curious about the smell of a cat and, instead of running away in self-preservation, stay in a place of high risk; the infection changes how they think and behave.
Multiple hits? Immune activation?
Dr. Postolache believes there is likely the need for at least a ‘double hit’ for suicide risk, and that the impact of multiple hits is more than just additive—it becomes exponential. So, in a person with an underlying mood disorder due to distal factors, the onset of allergy season and the resulting cascade of inflammatory cytokines may be enough to provide the proximal trigger that induces suicidal action. As in so many other health conditions, the issue at hand may be related to balance–with factors we rarely consider in mental health perhaps being responsible for tipping the scale towards suicide.
Dr. Postolache is interested in potential ‘upstream’ contributors that might contribute, either distally or proximally, in setting inflammatory pathways in motion to increase baseline or immediate risk of suicide. The factors currently under exploration are varied, and include microbes, pathogens, allergens, autoimmune conditions, medications, stress, diet, the microbiome, Vitamin D levels, oxygen levels, sleep, and traumatic brain injury.
Findings may assist in developing biomarkers, measurable risk factors, or treatments that can be tailored to an individual’s needs; Dr. Postolache reported on a study that revealed the positive effects of Vitamin D supplementation were only evident in those patients who were deficient to start. While the use of anti-inflammatory interventions has not been sufficiently explored to know if these might be effective in suicide, there is evidence of benefit in depression.
Dr. Postolache is a proponent of consideration of underlying biological conditions and treatments in the approach to mood disorders and suicide, as well as the opposite. Given overarching and related mechanisms and pathways in mind and body, and our knowledge that the vast majority of those who die by suicide have seen a medical doctor in the previous year, this quote from Dr. Erick Messias in The Atlantic article about Dr. Postolache’s allergy findings resonates: ‘We psychiatrists should pay more attention to the body, and people who pay attention to the body should pay more attention to the mind.’
Is activation of the immune system a key element that might turn a distal risk factor, such as early trauma or head injury, into heightened suicide risk? What else layers on additional risk? More importantly for treatment and prevention, what provides protection and fosters resilience? If we treat one of the hits, can we have exponential healing?
JKBF thanks Dr. Postolache for his presentation, but more importantly for his innovative thinking and exploration of novel questions. We wish him and his collaborators much success. We hope you will join us in helping to promote more investigations like these into the biological contributors to suicide.